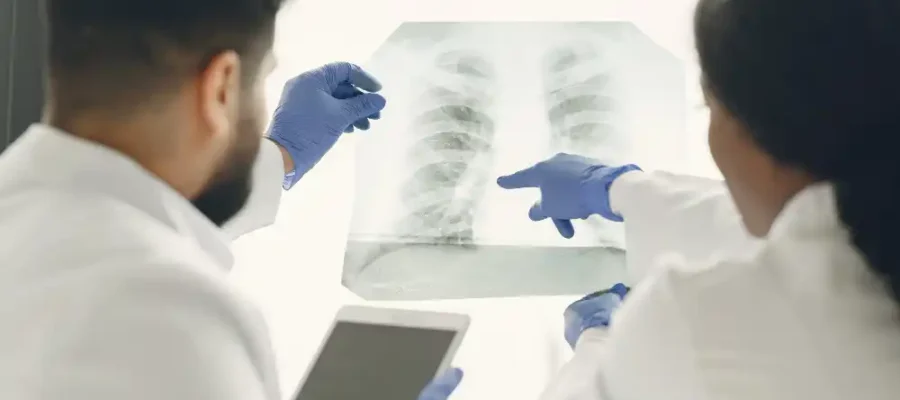
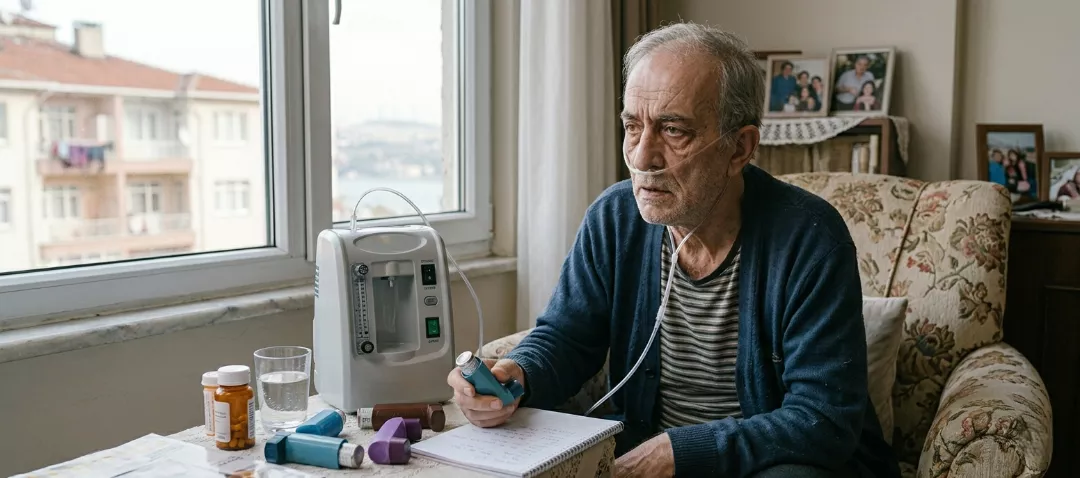
The question of whether breathing can become easier with COPD balloon treatment is raised very often, especially by patients who experience serious difficulty in daily life because of shortness of breath. Although COPD balloon treatment is not a standard procedure for every patient, it is considered among the interventional approaches that may help the airways function more comfortably in suitable individuals. When complaints such as difficulty breathing in and out, a feeling of pressure in the chest, quick fatigue, and reduced exercise capacity are present, COPD balloon treatment may become an option that supports quality of life for some patients. However, the most important point to understand is that this method is not a solution that completely eliminates the disease, but rather a procedure that may help increase breathing comfort in a specific group of patients.
The answer to the question of whether breathing becomes easier with COPD balloon treatment depends on the patient’s lung structure, the degree of airway narrowing, the extent of the disease, and the overall state of health. In some patients, once airflow becomes easier after the procedure, there may be less shortness of breath, less difficulty during daily activities, and more controlled breathing. On the other hand, in some patients the expected benefit may remain limited, or other treatment options may be more suitable. For this reason, the possible benefit of balloon treatment should not be determined by general information alone, but through a detailed evaluation, respiratory tests, and specialist opinion.
What Is COPD Balloon Treatment?
COPD balloon treatment is basically one of the procedures planned to evaluate narrowed or functionally impaired areas in the airways and, when appropriate, to relieve them through interventional methods. Here, the term “balloon” refers not to a structure that remains inside permanently, but to a medical tool that is used in a controlled way during the procedure and may help widen the relevant area. Although this method is sometimes thought of by the public as a treatment that opens the lungs or completely restores breathing, from a medical perspective it needs to be assessed more carefully.
COPD is not a single-type disease. In some patients, marked narrowing in the bronchial structure is the main issue, while in others emphysema, air trapping, chronic sputum production, or advanced lung damage may be more dominant. For this reason, balloon treatment is not performed in every COPD patient. If it is used, the goal is to support breathing, facilitate airflow, and contribute to quality of life in selected cases. The procedure is only one part of the overall management of the disease; medication, breathing exercises, smoking cessation, infection control, and rehabilitation remain just as important.
Why Can Breathing Become Easier with COPD Balloon Treatment?
One of the main reasons for shortness of breath in COPD patients is narrowing of the airways and difficulty expelling air from the lungs. Breathing becomes difficult not only when inhaling, but also when exhaling. Over time, this can lead to a feeling of fullness in the chest, air trapping in the lungs, and a marked sense of insufficiency during exertion. The reason balloon treatment may be beneficial for some patients is that it can provide mechanical relief in the airway and somewhat facilitate the passage of air. When airflow becomes more regular, the patient may begin to feel more in control of their breathing.
However, the feeling of easier breathing is not due only to physical widening. In some patients after the procedure, a reduction in chest tightness, a lighter cough burden, a decrease in the feeling of panic during exertion, and more efficient breathing also play an important role. Especially for people who struggle even while walking a few steps, climbing stairs, or speaking in daily life, even a small degree of relief can make a big difference. Still, the level of this effect varies from person to person. Therefore, the real measure of success is not simply that the procedure was technically performed, but whether it truly contributes to the patient’s breathing comfort.
In Which Patients Is More Benefit Expected?
The success of COPD balloon treatment is directly related to patient selection. The same method should not be expected to suit everyone who experiences shortness of breath. In some patients, the main problem is widespread lung destruction, while in others there may be more localized narrowing or structural problems that can be treated interventionally. This distinction is what determines who is more likely to benefit from the treatment. If the right patient is not selected, the procedure may fail to meet expectations; if the right patient is chosen, a meaningful improvement in breathing comfort may be seen.
Looked at briefly and clearly, the patient profile expected to benefit more may include the following features:
- Those who continue to experience marked shortness of breath despite medication
- Patients whose airway narrowing can be evaluated interventionally
- Those whose quality of daily life has significantly declined
- Individuals whose general health condition is suitable for the procedure
- Patients whose respiratory tests and imaging results support intervention
These points provide a general framework. The final decision, however, depends on the patient’s overall evaluation. This is because COPD is a chronic disease that does not progress only in the lungs, but can affect many areas, from heart health to muscle strength, and from nutrition to psychological condition.
What Can Patients Expect After COPD Balloon Treatment?
For most patients, the period after balloon treatment is at least as important as the procedure itself. This is because whether breathing has truly become easier usually becomes clearer not at the moment the patient leaves the procedure table, but in the days and weeks that follow. Some patients feel they can breathe more comfortably in the early period after the procedure, while for others it may take some time before a noticeable difference appears. The reason is that the lungs’ response, the accompanying condition of cough and sputum, and the overall breathing capacity vary from person to person.
After the procedure, mild coughing, a feeling of discomfort in the throat, short-term fatigue, or temporary changes in breathing may be observed. These do not always indicate something negative, but specialist follow-up is important. After treatment, the patient needs to pay attention not only to the interventional result but also to lifestyle. Continuing to smoke, using medication irregularly, failing to protect against infections, and neglecting breathing exercises can reduce the benefit gained. For this reason, the period after balloon treatment should be seen as part of a broader care plan that supports lung health.
What Are the Limitations and Risks of COPD Balloon Treatment?
When discussing COPD balloon treatment, it is not enough to describe only its positive aspects. As with any interventional method, there are limitations and risks here as well. One of the most important limitations is that the method does not completely cure COPD. Balloon treatment does not eliminate the progressive nature of the disease; it can only help relieve certain symptoms in suitable cases. In other words, even if it makes breathing easier for the patient, the need for regular follow-up and comprehensive treatment continues.
With a brief evaluation, the main points that require attention can be summarized as follows:
- Not every COPD patient is suitable for this procedure
- The expected benefit may remain limited in some patients
- Temporary coughing or changes in breathing may occur after the procedure
- There is a risk of infection, irritation, or complications related to the treatment area
- Risk assessment should be carried out more carefully in people with additional illnesses
These risks do not mean that the treatment is unnecessary. On the contrary, when it is planned in the right center, by an experienced team, and for the right patient, the procedure becomes safer and more beneficial. For this reason, medical suitability rather than emotional expectations should be prioritized during the decision-making stage.
Is Balloon Treatment Alone Enough to Reduce Shortness of Breath?
Although COPD balloon treatment may make breathing easier in some patients, in most cases it is not enough on its own. This is because COPD is a chronic disease that requires multifaceted management. Not only the narrowing in the airway, but also lung capacity, sputum burden, frequency of infections, physical condition, smoking history, and accompanying illnesses must be evaluated. Therefore, it is not realistic to expect a miracle from a single procedure. The best results are usually achieved when interventional methods are combined with regular medication and lifestyle adjustments.
In particular, pulmonary rehabilitation, controlled exercise, proper breathing techniques, weight control, nutritional support, and measures to protect against infections can all support the effect of balloon treatment. If the patient undergoes only the procedure but neglects the rest of the process, the benefit achieved may become limited in a short time. In contrast, in patients who are followed regularly, comply with the physician’s recommendations, and develop habits that protect lung health, breathing comfort may become more sustainable. Therefore, the real goal is not a single intervention, but the creation of a comprehensive respiratory management plan.
What Is the Most Realistic Answer to the Question of Whether Breathing Becomes Easier with COPD Balloon Treatment?
The most realistic answer to this question is this: Yes, COPD balloon treatment may make breathing easier in some patients, but this result is not seen at the same level in everyone. The success of the treatment depends on choosing the right patient, performing the procedure for the right indication, and maintaining the treatment plan afterward. Balloon treatment can be an option that provides serious relief in suitable individuals, but it may lead to disappointment if approached with the wrong expectations. For this reason, the method should not be evaluated with the idea that it is “good for everyone,” but through individualized medical assessment.
For COPD patients who have significant difficulty breathing, the most appropriate approach is not simply to look for a single procedure, but to identify the cause of the shortness of breath in detail. Sometimes the most appropriate option may be balloon treatment, sometimes other interventional methods may come to the forefront, and sometimes the greatest benefit may be achieved through medication adjustment and rehabilitation. As a result, although COPD balloon treatment is an important option with the potential to make breathing easier in the right patient, real success is only possible with a personalized treatment plan.