COPD often presents with subtle symptoms in its early stages; for a while, people tend to brush them off as “seasonal changes,” “the effects of smoking,” or “I guess I’m just getting older.” Yet COPD (Chronic Obstructive Pulmonary Disease) is a condition that can be managed more effectively when caught early, with exacerbations reduced and quality of life significantly improved. So the issue is not only getting a diagnosis; it is getting that diagnosis early and establishing the right routine.
In fact, knowing the early symptoms of COPD is valuable not to “be afraid,” but to “take control.” It should also be remembered that early-stage COPD symptoms are often mild, but persistent. We can sum it up like this: if you learn to read your body’s small warnings correctly, you are investing in your breathing.
What Is COPD And Why Are Early Symptoms Important?
COPD is a respiratory disease characterized by narrowing of the airways and damage to lung tissue, and it may progress over time. One of its most important features is that, in the beginning, it can feel “tolerable.” And that is exactly what misleads people. Because a person goes about daily tasks, gets briefly short of breath, coughs now and then, and says, “It’s normal.” Then one day, they begin stopping to catch their breath while climbing stairs; that is the day awareness starts to rise.
Why is the early stage so critical? Because the steps taken during this period—quitting smoking, establishing the right medication routine, preserving exercise capacity, reducing exacerbation risk—make the course of the disease more manageable. Among the most common symptoms of COPD are complaints such as shortness of breath, chronic cough, sputum, and fatigue.
Symptom 1: A Persistent Cough
One of the most typical early signs of COPD is a long-lasting and “stubborn” cough. This cough may not continue all day; it may be more noticeable in the mornings and ease during the day. And that is exactly why people are misled: “It only happens in the morning, I must have caught a chill.” So after how many weeks does it stop being “normal”? Instead of focusing on an exact number of days, it is more accurate to ask: does the cough keep coming back, has it become almost like a habit, has it quietly settled into your life without you noticing?
And a cough has its own language. Is it dry and irritating? Or is it a chesty, “full” cough? In COPD, what is often seen is a chest-originating cough that may come with sputum.
It should also be remembered that in people who smoke or used to smoke, a cough labeled as a “smoker’s cough” can sometimes be an early signal of COPD. Changing the name does not change the reality; a cough is still a cough. And if it is becoming chronic, it needs to be taken seriously.
Symptom 2: Increased Sputum And Morning Congestion
The issue of sputum is generally underestimated. Because people tend to normalize it with thoughts like “everyone has some sputum.” Yet in the early stage of COPD, sputum can become regular: especially the need to clear the throat in the mornings, a feeling of fullness in the chest, producing more sputum during the first hours of the day… these are important signs.
The color and consistency of sputum also offer clues. Clear or whitish sputum may be associated with chronic irritation and increased secretions. Turning yellow-green or a marked increase in amount may suggest conditions such as infection or an exacerbation. Rather than judging based on a single day, it is healthier to look at the “change”: if it was not like this before and has started becoming this way, it should be noted.
In fact, increased sputum can be thought of as the airways’ way of protecting themselves. But if that reflex is constantly active, there is a reason. It is easy to say, “That is just how my body is,” but in the long term, the cost can be high.
Symptom 3: Shortness Of Breath With Exertion
In the early stage of COPD, shortness of breath usually appears only with exertion. In other words, not while sitting; but while walking, climbing uphill, talking quickly, carrying shopping bags… That is why people think, “I’m just out of shape.” Yes, your fitness can decline; but if shortness of breath has become regular, saying it is only fitness can sometimes mean missing the bigger picture.
Ask yourself this question: which task that used to be easy for you has now become harder? Stairs, brisk walking, household chores? Among the common symptoms of COPD, experiencing shortness of breath during daily activities is clearly included.
It should also be remembered that in COPD, shortness of breath does not appear “in one day”; it increases gradually. It is easy for a person to get used to it, and hard to notice it. But that is exactly why observing yourself in the early stage is so valuable.
Symptom 4: Wheezing, Chest Tightness, And Feeling Unable To Take A Deep Breath
Some COPD patients feel a fine whistling sound—like a wheeze—when they breathe. Sometimes only you notice it, sometimes people around you say, “Your breathing sounds noisy.” Chest tightness, pressure, and the feeling of “I can’t take a deep breath” may accompany this group of symptoms. These symptoms may come and go; in other words, they may not be equally intense every day. But if they keep recurring, the message is clear: the airways are not comfortable.
The feeling of not being able to take a deep breath can sometimes be confused with anxiety. A person may think, “I got panicked,” when in fact the body is already struggling. Of course anxiety affects breathing; but labeling it only as “psychological” can be risky. Because in COPD, wheezing and chest tightness are among the complaints that can be seen in the early stage.
Here is a small clue: if these complaints increase especially in cold weather, dusty environments, or with perfume/chemical smells, airway sensitivity is involved. And that deserves evaluation.
Symptom 5: Frequent Infections And Prolonged Colds
In the early stage of COPD, frequent “chest infections” or prolonged colds are also important signs. A cold that you would normally recover from in a week may last two weeks this time. Or you may feel that it “goes to your chest” several times every winter. Frequent infections may indicate that the defense system of the airways is under strain.
This picture may also increase the risk of exacerbations. What we call an exacerbation is a clear worsening of COPD symptoms that disrupts the daily routine; sometimes it requires additional treatment. Respiratory tract infections occupy an important place among the triggers of exacerbations.
It should also be remembered that “frequent infection” is not only about immunity; environment, cigarette smoke, air pollution, sleep irregularity, stress… all can feed into the picture. So here too, a systems-based approach is needed.
Why Symptoms Start Slowly: The “I’m Just Getting Older” Misconception
The biggest reason COPD is missed in its early stage is that the symptoms increase gradually. People get used to the change. Yesterday you were climbing 10 floors, today you stop and rest at the 8th… you say, “Normal.” A month later you are down to 6 floors… still “normal.” Yet that normalization can sometimes mean turning a blind eye to the silent progression of the disease.
Another misconception is, “Everyone coughs in winter.” Yes, they do. But is yours the same every winter, the same every morning, a little worse every year? That is where the difference lies.
In fact, the main idea of this section is this: do not expect a dramatic beginning in COPD. The persistence of small signals is the most important clue.
Most Critical Question 1: How Can COPD Be Distinguished From Asthma Or A Simple Smoker’s Cough?
- Look At The Timeline: COPD usually develops slowly over the years and comes with persistent complaints; asthma, on the other hand, may fluctuate with attacks in many people.
- Note The Triggers: In asthma, sudden narrowing may be more prominent with triggers such as allergens, exercise, or cold air; in COPD, a lasting decline in daily exercise capacity may stand out.
- The Character Of The Cough Matters: A morning cough and sputum that are dismissed as a “smoker’s cough” should raise the possibility of COPD if they have become regular.
- Night Waking And Tightness: Nighttime shortness of breath can occur in both conditions; but the combination of sputum, cough, and exertional breathlessness strengthens the need for evaluation.
- Definitive Distinction Is Made By Testing: The clearest distinction is made with pulmonary function tests (especially spirometry) and a physician’s assessment; “I felt it” is not enough on its own.
We can sum it up like this: labels create confusion, measurement brings clarity. What matters is not naming the complaint, but identifying it correctly.
What Happens During The Diagnostic Process: Spirometry And Other Steps
When COPD is suspected, the most basic evaluation is the pulmonary function test. People commonly call it a “breathing test”; you blow in a certain way, and it measures how the lungs manage airflow. This test helps determine the presence and degree of airway narrowing. The picture is then completed with examination, medical history (smoking history, occupational exposure, indoor smoke, childhood infections), and, if necessary, additional tests such as imaging or blood work.
There is an important point here: you do not have to be in very bad shape to be diagnosed with COPD. Going for an evaluation in the early stage means “not waiting for things to get worse.” Many people say, “I wish I had gone earlier.” Because in the early stage, the impact of the right steps is more noticeable.
In addition, your doctor will evaluate exacerbation risk, accompanying diseases, the medication plan, and lifestyle adjustments together when needed. So this process is not the result of a single test; it is a comprehensive evaluation.
When Should You See A Doctor Without Delay?
- If Your Shortness Of Breath Is Increasing Rapidly: If there is a clear worsening compared to your normal days, saying “I’ll wait, it will pass” may not be the right choice.
- If There Is A Sudden Change In Sputum: Increased amount, darker color, thicker consistency; especially if accompanied by fever or palpitations, this is important.
- If There Is Severe Chest Tightness Or Increased Wheezing: If you are too short of breath to speak comfortably, evaluation is necessary.
- If You Can No Longer Do Daily Tasks: The same stairs, the same walk… but now you cannot manage them, that is a signal.
- If You Have Frequent Infections: Especially if chest infections that last long and recur during winter are happening repeatedly.
- If You Experience Bluish Lips, Confusion, Or A Fainting Sensation: Findings like these may require urgent evaluation.
It should also be remembered that the sentence “something just doesn’t feel right” is also a sign. You know your own normal best.
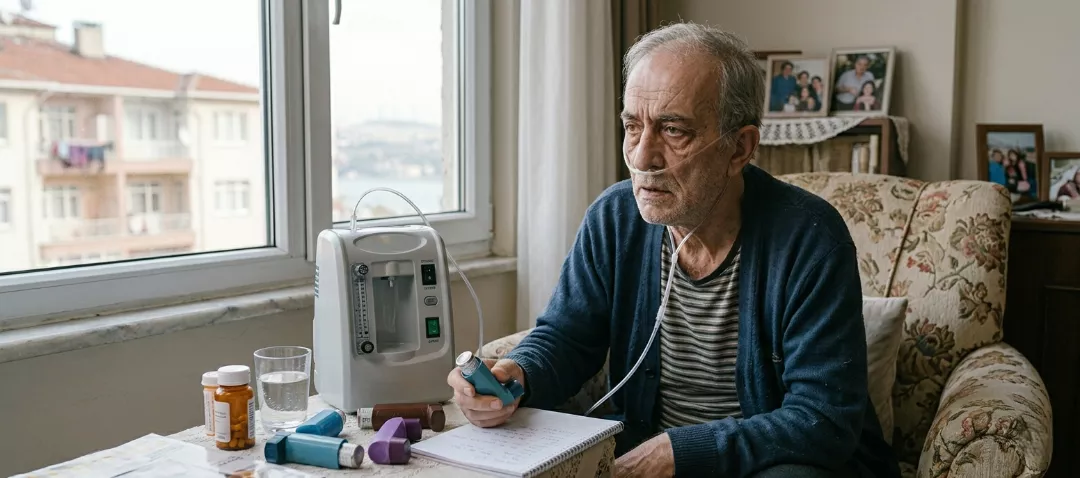
Smart Steps You Can Take In The Early Stage
Let’s say you noticed the early symptoms; what next? The goal here is not panic, but a plan. The first and strongest step is quitting smoking if you smoke; if you do not smoke, reducing exposure to smoke and polluted air. Even reducing scented chemicals inside the home, establishing a ventilation routine, and lowering dust exposure can ease breathing in some people.
The second step is not giving up movement completely. When shortness of breath becomes frightening, people want to stop; but as muscles weaken, the same task becomes harder. Controlled walking, simple breathing exercises, and programs prepared with professional support when needed may help preserve capacity. I am not saying “push yourself”; I am saying “do not abandon yourself completely.” A subtle difference, a big result.
The third step is recognizing exacerbation triggers. In which season do you get worse, in which environment does the cough increase, with which smell does wheezing begin? Taking notes on these will also strengthen your doctor’s evaluation. Because concrete data speeds up the process.
The fourth step is taking sleep and nutrition seriously. Fatigue and weakness can be seen in COPD; this also reduces activity. Good sleep and balanced nutrition—I will not call them “medicine,” but they truly are supportive.
The fifth step is going to follow-up visits regularly and, if an inhaler is prescribed, learning the technique correctly. Because the right device can be wasted with the wrong technique. Sometimes a small correction like “inhale this way” can change your whole day.
Common Mistakes In Daily Life
The most common mistake I see in people experiencing the early symptoms of COPD is underestimating the symptoms. “There’s nothing wrong with me, I’m just a little short of breath.” That “little” can grow over time. Another mistake is expecting medication alone to solve everything. Medication matters, yes; but without factors such as air quality, movement, sleep, and exacerbation management coming into play, control becomes harder.
Another mistake is turning to self-directed treatment: unconscious use of antibiotics, random use of bronchodilators, herbal mixtures recommended by neighbors… these can sometimes cause delay. It should also be remembered that COPD management is individualized; the same complaint may not mean the same thing in two different people.
Finally, stopping everything on the “good days.” Good days are actually the best days to establish a routine. Not when things get worse; the system needs to be built while things are still going well.
Knowing The Early Symptoms Means Protecting Your Breath
The 5 early symptoms of COPD—persistent cough, increased sputum, shortness of breath with exertion, wheezing/chest tightness, and frequent infections—usually begin slowly and are easily normalized. But if these symptoms have become persistent, especially in people with a smoking history or a story of heavy exposure, getting evaluated is a smart step.
In fact, the clearest message of this article is this: recognizing COPD early is not about “being afraid”; it is about having the chance to live better. We can sum it up like this: if your breathing is trying to tell you something, listen. Because the right steps taken in the early stage can affect even the years ahead.